Surgery |
||
Leg splint (1) |
||
Already the antique knew greaves of metal. In the Middle Ages, the leg was wrapped after repositioning of the bone [with a screw clamp] with strips of linen, were glued to the wood chips in the longitudinal axis of the leg. These chips were then lashed together with knitting to hold the bone fragments.
|
Surgery |
||
MAYOR leg splint (2) |
||
"An advancement in the field of flexible splints was the wire mesh introduced in 1836 by the Swiss surgeon Mathias Louis MAYOR (1775-1847) as well as the telegraph wire splint by ESMARCH, which is the archetype of our" empty splint.
"The Cramer rail was developed in the 1980s by the Wiesbadener surgeon CRAMER (died 1903) stated "(Mrs. Härtel, Mrs. Loeffler The Association: Textbook of Surgical and Orthopedic Association Treatment, Berlin 1922 P. 74).
|
Surgery |
||
Leg splint (3), wooden |
||
When a Tyrolean mountaineer had broken his foot - the Tyroleans say "to Hax åkrissn" - he had to be carried on the hump of a helper or in the basket to the valley. Even today, a foot or a leg must be immobilized if the transport does not degenerate into nightmare and the damage to tapes and vessels should be even greater than they are anyway.
|
Surgery |
||
Lenticular |
||
This instrument is doubtless a lenticular (originally I took it for a tartar remover), comes from an antique shop in Innsbruck.
Here the description of the instrument in the "Dictionnaire des sciences médicales, Paris 1818":
... a rasp used in ancient neurosurgery. Therefore, you will find similar devices under the name "raspartoire" or "râpe". In France they were later called "rugine". The "lenticular", as the English call it, was round-headed, but also, as in the present case, a pentagonal head, the tip of which was turned towards the surgeon, but whose rounded lower edge was pressed against the meninges, an injury the same while the 4 side edges smoothly rasped the bony edges of the trephination site.
The lenticulars were found in trepanning utensils until around 1920, when they gradually disappeared from the company's offer. The "Berlin Waarenhaus" offered around 1910 none more, but the Fa. Esculape, 1910 by P.J. Mountain, Grossstrasse 17. |
Surgery |
||
Military helmet |
||
In 1914, the armies went over to the war of position, from the beginning of 1915, they began to prepare for infantry attacks by hours of artillery fire. It was mainly used shrapnel and shrapnel projectiles, which unfolded a devastating effect on humans. Within a short time, the proportion of wounds increased massively. About a quarter of these wounds were head injuries and thus almost always fatal. So it was hurry to protect the heads of the soldiers.
The German helmets M1916 / M1917
The inventors were three people. Since both technical and anatomical problems were to be solved, the cooperation of several people was required - Friedrich Schwerd (1872-1953), who was a professor at the Technical University of Hannover, in the war captain of the Landwehr;
The typical American helmet M1
|
Surgery |
||
Needle box (1) |
||
Needle boxes (square) for sterilizing and storing sewing needles. Sliding lid / hinged lid.
|
Surgery |
||
Needle holder (1) |
||
|
Surgery |
||
Needle holder (2) |
||
Three men have made a special contribution to seam technology: - Jacques-Louis REVERDIN (1842-1929) from Geneva, who had been trained in Paris - who in 1879 published a paper on a modification of the needle of the tub BRUNNS: the pedicled needle "à chat mobile" was born.
- Auguste REVERDIN (1848-1908), cousin of the former, had been trained in Strasbourg, in 1887 he gave a needle holder "à pédale" with interchangeable needle. His son
- Albert REVERDIN / 1881-1929) improved the instrument even further. Since he worked at the hospital in Lausanne for a while, we tend to see Georges-Louis GAUDIN co-inventing the needle holder.
Jacques-Louis Reverdin (1842-1929) Cette aiguille est modifiée par la suite par son cousin le sur les Auguste Reverdin (1848-1908) et son neveu le Surgeons Albert Reverdin (1881-1929) ". *** I could not find out anything reliable about GAUDIN. - Dr. Georges Louis GAUDIN (1821-1875) was from 1866 established as a surgeon in Lausanne. - Dr. Célestin Philippe GAUDIN (1818-1879) .Maire de Saint-Georges-de-Didonne de 1871-1874. Il est né en 1818 à Marennes et il est mort le 9 avril 1879 à SGD. Il était alors Surgery Major de Marine en retraite et consultant à VICHY. Il était chevalier de la Legion d'Honneur le 16 septembre 1860 et chevalier de l'Ordre Suédois de Wasa de 1869. Il a écrit de nombreux ouvrages de médecine, e.a. "Traité d'hygiène navale". Célestin-Philippe-Baptiste Gaudin, soutint à Montpellier en 1861 une thèse intitulée «De l'heureuse influence du climat de l'île de la Réunion et des eaux thermales de Salazie sur la guérison de la cachexie paludéenne». Il écrivit avec Louis Alexandre Petit, Médecin de la Marine en poste à la Réunion de 1855 à 1861 en tant que directeur de Service de santé, un guide intitulé «Guide to the medical and technical services of Salazie, île de la Réunion. Saint-Denis (Réunion), 1857, Vilal Delval, 1 vol. in-8, avec 6 lithographies ».
|
Surgery |
|||
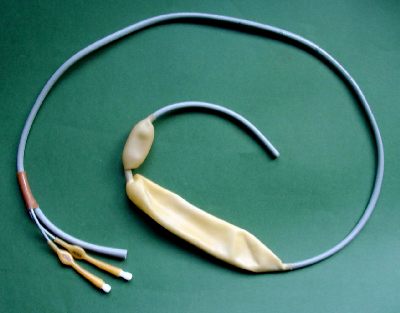
Oesophagus, dilatator by SENGSTAKEN-BLAKEMORE |
|||
Patients with cirrhosis of the liver are interned patients for years, so even in case of emergency, they primarily turn to their internists: they even come to the Internist Outpatient Clinic, even with massive bleeding from esophageal varices (a classic result of liver cirrhosis), and the first measures have to be taken by internists.
|
Surgery |
|||
Oesophagus, probe 2 |
|||
Long flexible metal probe, with a screw-on ivory olive on top, with holes in the esophagus (tumor lining, obstruction due to scarring) boughened.
- Hôpital TROUSSEAU in Paris XIIe arrondissement; 26, avenue du Docteur Arnold-Netter. |
Surgery |
||
Oesophagus probe (part 1) |
||
"Foreign bodies in the esophagus are often the opportunity for surgical intervention, one must try to extract them with suitable instruments," coin catcher ", etc., or push them down into the stomach, only in desperate cases do they proceed to the opening of the esophagus Esophagotomy (Greek: esophagotomy) by opening the esophagus from the outside through the skin and muscles of the neck.This operation is difficult and not dangerous, it is also performed if, after sulfuric acid or alkali poisoning or following cancerous destruction, such narrowing of the esophagus that even fluid food does not even get into the stomach and death threatens by starvation "(Meyers Konversationslexikon, 4th ed. 1892).
Armand TROUSSEAU (1801-1867) was once considered the greatest clinician in France. In Paris he performed the first tracheostomy for Krupp. While suffering from asthma, in 1844 he developed cigarettes whose active ingredients were used to treat the seizures - the method was practiced until 1995.
TROUSSEAU proposed a set of extension olives to cure narrowing of the esophagus. Interesting is next to the ivory olives the coin catcher "crochet à bascule de GRAEFE", a kind of small parachute, with the swallowed coins could be pulled up ...
"Ulflingen, Sept. 28 (Rescued) The 5-year-old son of a station assistant stationed there recently played with a coin.As usual for the children, the little one took the coin in his mouth and suddenly swallowed it in the esophagus, where it was swallowed During this time the child was unable to eat solid food and suffered great pain, until the medical art and skilful treatment of Mr. Delvaux of Luxembourg succeeded in taking out the coin now happy and cheerful again "(Bürger- und Bürgertenzeitung of 1.10.1903).
Illustrations of the coin catcher can be found p. 212/213 in the edited in 1910 (1987 re-published) Catalog of "Medicinisches Waarenhaus Action Society Berlin". |
Surgery |
||
Patient transport (1914/18) |
||
Ambulance done by the Nürnberg "Spielzeugfabrik Georg Fischer in the 1930th years |